The Haven
Healing Centre
The Orchard
Draycott Rd, Cheddar
Somerset

The Haven |

|
| Natural Complementary Therapies - your key to improved health and well-being | |
|
Home About Contact Gift Solutions Articles Treatments Products Page: 1 2 3 4 5 Appointments |
Achilles Tendonitis (Tendinopathy) TreatmentAchilles tendinopathy is a common cause of disability in sportAchilles Tendinitis, or Tendon Rupture are the bane of many runners, and is a common sporting injuryWhat is Achilles Tendonitis? Achilles tendonitis is a painful condition of the tendon in the back of the ankle, and left untreated, can lead to an increased risk of Achilles tendon rupture. It is estimated that achilles tendonitis accounts for around 11% in runners, 9% in dancers, and just under 2% in tennis players. The condition is not only restricted to athletes though, as 25% to 30% of those affected are non-athletes who may lose significant numbers of workdays while in recovery. The Achilles tendon is the large tendon at the back of the ankle. It connects the large calf muscles (Gastrocnemius and Soleus) to the heel bone (calcaneus) and provides the power in the push off phase of the gait cycle (walking and running). Tendonitis is inflammation of the tendon, usually resulting from overuse associated with a particular playing surface, improper footwear, misalignment, or intensity of an activity. The Achilles tendon is surrounded by a connective tissue sheath and does not have a good blood supply, lubrication or cell activity, so this injury can be slow to heal. The tendon receives nutrients from the tendon sheath or paratendon, which stretches with movement, allowing maximum gliding action. When an injury occurs to the tendon, cells from surrounding structures migrate into the tendon to assist in repair. 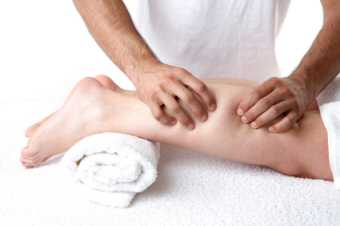 Some of these cells come from blood vessels that enter the tendon to provide direct blood flow to increase healing. With the blood vessels come nerve fibers, which may be the cause of the pain.
Some of these cells come from blood vessels that enter the tendon to provide direct blood flow to increase healing. With the blood vessels come nerve fibers, which may be the cause of the pain.Treatment Seek professional advice and treatment as soon as possible, because this injury can lead to an Achilles tendon rupture with continued overuse. Treatment options vary, but expect to hear about things like, ice, cold compression therapy, non-steroidal anti-inflammatory drugs (such as ibuprofen), ultrasound therapy, manual therapy techniques (like sports massage), a rehabilitation/exercise program, and in rare cases, application of a plaster cast. A raised heel pad is sometimes used to take some of the strain off the achilles tendon, but this should only be a temporary measure. If you can avoid it, do so. An exercise routine should be designed to strengthen the tendon, not wear it out even more, and patients advised not to 'push on' with ever more demanding stresses, as a treatment program can mask the early pain signals that can increase the risk of tendon rupture. Achilles tendonitis is a condition of irritation and inflammation of the large tendon in the back of the ankle and so can lead to pain and swelling. Furthermore, Achilles tendonitis can lead to small tears within the tendon, and make it susceptible to rupture. Long distance runners, and short burst sports people, like rugby and football players, can have symptoms of Achilles tendonitis after making abrupt changes to mileage and training or footwear. As we grow older, tendons, like other tissues in the body, become less flexible, more rigid, and more susceptible to injury. Adults can become worried about their general health and begin exercise programs that may be classed as 'Too much, too often', making them susceptible to Achilles tendonitis. What are the symptoms of Achilles tendonitis? Achilles tendonitis, now often referred to as achilles tendinopathy,  is usually found to be degenerated tissue with a loss of normal fibre structure around 3-6 cms up from the heel, but may also originate from the tendons attachment point on the heel.
It may be associated with inflammation, redness, swelling and a thickening or hardness which will be tender on palpation. There may also be nodules or lumps in the tendon, but these may only be evident upon a reduction of swelling/oedema around the base of the tendon. The main complaint associated with Achilles tendonitis is pain over the back of the heel. Pain can be either acute (occurring over a period of a day, or a few days), following a sharp increase in training, or chronic which occurs over a longer period of time (weeks, or even months).
is usually found to be degenerated tissue with a loss of normal fibre structure around 3-6 cms up from the heel, but may also originate from the tendons attachment point on the heel.
It may be associated with inflammation, redness, swelling and a thickening or hardness which will be tender on palpation. There may also be nodules or lumps in the tendon, but these may only be evident upon a reduction of swelling/oedema around the base of the tendon. The main complaint associated with Achilles tendonitis is pain over the back of the heel. Pain can be either acute (occurring over a period of a day, or a few days), following a sharp increase in training, or chronic which occurs over a longer period of time (weeks, or even months).Patients with Achilles tendonitis usually experience the most significant pain after periods of inactivity and often they complain of pain on taking their first steps in the morning, or after sitting for long periods. Pain often fades with the onset of exercise, but may return when running, jumping or pushing off with force. Chronic achilles tendonitis is the most likely outcome from acute tendonitis if it goes untreated for any length of time. With chronic tendonitis the pain will become fairly constant, and hills or stairs increasingly difficult. Unfortunately, for the average older athlete, a chronic tendonitis condition will be more difficult to treat, will occur more often, and with less reason. Occasionally an MRI scan is performed to evaluate a patient for tears within the tendon, or to prepare a patient for preoperative evaluation and surgery planning, where that is the most likely outcome. Causes and Outlook for Achilles Tendonitis Achilles tendonitis is an overuse injury, plain and simple. Sports therapists state this as: Too Much, Too Soon, Too Often. If you treat this injury early enough you should make a good recovery. The worst thing you can do is ignore it or try to run it off. Post healing rehabilitation will ensure the tendon properly heals and strengthens. Failure to do this effectively will leave the tendon weaker than normal and will likely cause the injury to return, even worse than before. If you ignore the early warning signs it may become chronic which will be very difficult to treat. So what's this story you are talking about? - Six Months of Hell - An Achilles Tendonitis Case Study This story is about a patient who suffered a gradual increase in pain and disablement over a month, starting about six months ago. She was not athletic, but did have a cleaning job that required a certain level of fitness. A visit to the doctor produced a prescription for some NSAID's (Non-steroidal anti-inflammatory drugs) and advice about bedrest. The problem remained and so she went back. This time a course of physio and some topical pain relief cream was prescribed. Still no good, so an ultrasound followed, and then a steroidal injection which later caused a sharp increase in pain and a reduction in use of the foot. So much so, that now the patient couldn't even walk up or down stairs and had to take several weeks off work to rest. Early morning pain and stiffness meant it became more and more difficult to face the day. Strapping didn't work, neither did changes to footwear, working practices or pain killers. The patient became depressed and worried that there would be no end to this problem, even paying privately to see a consultant in the hospital, who told her she may have to put up with this for the rest of her life. Actually, the doctor said this at some point during one of the visits, but she didn't register it until the second statement drove it home. During her time in hospital, she received an MRI and more physio, but was released when the test were completed. The recommendation was, more rest. The thing I find most bizarre about this whole sorry tale, is that at no time did anybody actually touch her ankle, or indeed ask her to take her sock off, except to do the scans. In sheer desperation, following the recommendation of a friend she rang to ask if there was anything I could do. Bear in mind that I had no knowledge of the previous treatments when she showed up at my clinic. On examination (yes, actually palpating the injured area), I figured that this was a classic case of achilles tendonitis. 'Oh yes,' she said, 'One of the doctors said it was that, but I didn't know what it was and I was afraid to ask. He just wanted me out of the surgery'. I refrained from saying anything I would probably have regretted after, and proceeded to treat her ankle.  The ankle, by this time, was severely swollen and painful to touch. However, I began by performing very light strokes and used a technique called
Manual Lymphatic Drainage (MLD), to try to reduce the swelling. As the tightness in the ankle began to subside and the skin began to move more readily, I applied a little ice pack to accelerate the drainage of the ankle, which I continued to monitor for about 15 minutes. At the end of that time I could palpate the achilles and even make out an outline of the tendon, even if I couldn't grasp around it. I used some
Sports Massage techniques, modifying them so as to work very lightly, in an effort to allow access through the tissue to the tendon.
The ankle, by this time, was severely swollen and painful to touch. However, I began by performing very light strokes and used a technique called
Manual Lymphatic Drainage (MLD), to try to reduce the swelling. As the tightness in the ankle began to subside and the skin began to move more readily, I applied a little ice pack to accelerate the drainage of the ankle, which I continued to monitor for about 15 minutes. At the end of that time I could palpate the achilles and even make out an outline of the tendon, even if I couldn't grasp around it. I used some
Sports Massage techniques, modifying them so as to work very lightly, in an effort to allow access through the tissue to the tendon.It was obvious that due to inaction, this condition had become chronic and would be difficult to treat effectively, but gradually, I was able to increase the pressure of the massage strokes by which time the swelling around the tendon and ankle was almost gone. Once I was happy with the shape, I strapped an ice gel pack to either side of the tendon, wrapped them in cling film and told her to come back in two days. On the way out to the car, I recommended she ice for 20 mins, refreeze the packs for 2 hours and ice again, doing this for the rest of the day until bedtime. She came back two days later, with the ice packs, and told me how that evening she was pain free for the first time in 6 months. She was so excited that she did the hoovering, the dusting, two loads of ironing, made the beds and basically cleaned the house from top to bottom. Realize that wasn't my recommendation, nor part of the deal, but this gives an idea of how desperate some people become when they are incapacitated for so long. She said, 'I so wish I'd come before. All I could think of was, WHY DID I WAIT 6 MONTHS??'. Of course, by the second day of feverish activity, the pain had returned and so we did the whole routine again. I did recommend that she moderate her workload so as to not aggravate the problem and to allow time for the tendon to repair and start producing its own lubricant. Now, we are several weeks later and the pain has not returned, and normal duties have been resumed. So why did this work so well? I think it has to do with the multi-disciplinary approach. All too often, we are offered drugs that knock you sideways, or specialist therapy (like physio) that suffers from a bit of tunnel vision. If the therapy doesn't work, it must be the patients fault. At the same time, the 'old school' physio seems to be dying out in favour of this 'no hands' modern approach, which isn't very effective and leaves patients frustrated with the experience. I'm a great believer in physical, hands on, therapy. Touch and heal. Palpate around until you understand the problem and use that process to tell the brain that this is where you send the fix. By bringing in training from one therapy and marrying that to techniques from another therapy, you get to use the best of your arsenal in a joined up way. This I feel brings benefits to the patient that just aren't possible in a single discipline practice. My message to you is simple. Even if everyone around you is willing to give up; let them. Just you make sure, YOU DON'T GIVE UP! If you think you've tried everything and nothing has worked so far, look elsewhere. If this idea resonates with you, I invite you to visit The Haven Healing Centre in Cheddar for a course of treatment. Appointments and a treatment price list are available by clicking here. I look forward to welcoming you soon. Phil. Please share this page with your friends. Thank you.
Note: DISCLAIMER: This information is not presented by a medical practitioner and is for educational and informational purposes only. The content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read. It's a small investment in yourself, but could be a life-changing experience you will cherish forever. |
| Copyright © Philip Chave 2008- TheHavenHealingCentre.co.uk All rights reserved. Email: privacy |